Indian Journal of Health Social Work
(UGC CARE List Journal)
A REVIEW ON THE SWAY OF INFERTILITY ON THE MARITAL SATISFACTION OF COUPLES
Sreemol Sunil1 & Anish K.R.2
1Ph.D. Scholar, Rajagiri College of Social Sciences, Kalamassery, Kerala, India, 2 Assistant Professor, Rajagiri College of Social Sciences, Kalamassery, Kerala, India
Correspondence: Sreemol Sunil, e-mail id: sreemolsunil@gmail.com
ABSTRACT
Background: Infertility is a complex issue that affects individuals and groups, and also it has serious implications for the mental well-being and marital relationship of those involved. It is being recognized as a health issue worldwide. Aim: This review is to assess marital satisfaction in the context of infertility, using data from infertile individuals or both couples. Methods: This study is a scoping literature review of research studies conducted on factors associated with marital satisfaction and well-being in infertile couples. The current literature review search was undertaken using multiple databases selected from articles pertinent to the study. The selection of subjects was undertaken from 2000 to 2019. Results: A total of 623 papers were retrieved, plus the 7 articles from the author search. 6 more studies were identiûed by going through the reference lists of the selected papers and conducting an author search. Finally, 17 articles were included in this review. Conclusion: The results of this review article depicted that the sway of infertility on couples lead them to a lower state of marital satisfaction. The review showed evidence that infertility has a negative effect on the marital satisfaction and sexual relationships of couples, the stresses associated with infertility and related treatment had a negative impact on marital quality. It was identified that infertility, regardless of which gender experiences it, brought along many problems such as unhappiness, stress, losing privacy of sexual life, having sexual intercourse. Infertility and its treatment have effects on marital relations and Quality of life. The effects varied depending upon the stage of infertility process, gender, and the quality of the relationship. The studies also verify that infertile couples are in need of psychosocial interventions; thus, establishing a need for psychosocial interventions.
Keywords: marital satisfaction, sexual satisfaction, marital relationship, infertile couples.
INTRODUCTION
Infertility has become complex issue that affects individuals, society and groups in different cultures. It is being recognized as a health issue worldwide. According to the World Health Organization (WHO), sterility and infertility will become the third most serious disease worldwide after cancer and cardiovascular diseases in this century. Infertility is “a disease of the reproductive system defined by the failure to achieve a clinical pregnancy after 12 months or more of regular unprotected sexual intercourse” (WHO-ICMART, 2013) Infertility can lead to major social, emotional, mental disorders, as well as a reduction in satisfaction of marital life and quality of life (Masoumi et al, 2016). In developing countries, infertility is one of the most important and underappreciated aspects among reproductive health problems. Prevalence of Infertility was found to be highest in South Asia, North Africa/Middle East, Sub-Saharan Africa and Central/Eastern Europe and Central Asia. As per this research the absolute number of couples affected by infertility increased from 42.0 million
METHODOLOGY
The study is a literature review on the sway of infertility on the marital satisfaction of couples. A comprehensive search was conducted of the electronic databases of PubMed, EBSCO and google scholar for papers published in English between 2000 and 2019 that focused speciûcally on the effect of infertility on couples, including men and women. The keywords that were searched included: infertility OR infertile couples OR childless couples AND marital OR sexual relationship OR marital satisfaction AND sexual satisfaction AND infertility interventions.
A total of 623 papers were retrieved, plus the 7 articles from the author search. 6 more studies were identiûed by going through the reference lists of the selected papers and conducting an author search. Finally, 17 articles were included in this review.
Studies were included in the review if they met the following criteria: (a) were published in peer-reviewed journals; (b) presented original ûndings;
(c) The primary or secondary objective was to assess marital relationship or satisfaction in the context of infertility. (d) were articles published between 2000 and 2019. (e) The study participants comprised of infertile couples, or infertile individuals. (f) A validated, relevant instrument was used to assess marital satisfaction. Furthermore, studies without original data. reviews, debates, case reports, editorials, meeting abstracts non-peer-reviewed articles and brief communications were excluded.
Extraction of data
Initially, the titles and abstracts succeeding the search strategy was evaluated and eligible studies were selected. Certain studies were omitted at this phase as they were scarce of evidence with regard to the inclusion criteria. Secondly, the full-text of selected studies were further evaluated to
decide whether they fulfilled the inclusion criteria. Quality assessment of the studies were done to meet the research questions. The criteria for evaluating the quality of studies included in our study were: the quality of the measure instrument, the profile of study participants, study design and main results.
RESULTS
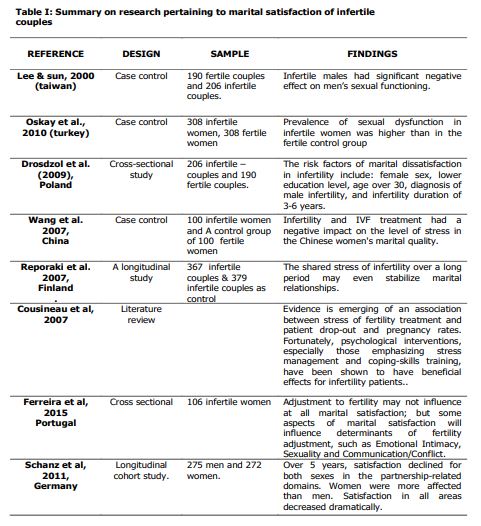
Characteristics of The Selected Studies
All of the 17 studies included in this review were published in peer-reviewed journals published between 2000 and 2019. There were 10 cross-sectional studies, 3 case control studies, 1 qualitative study using in-depth interview, 2 longitudinal studies and 1 literature review. The identiûed studies represent a diverse population from 12 countries, with seven studies conducted in Europe (Germany, Turkey, Finland, Portugal, California and Poland). Eight from Asia (China, India, Korea, Jordan, Taiwan) and one from Africa (Egypt). The literature focused on two aspects marital satisfaction and the need for interventions pertaining to infertile couples. Of the 17 studies, 7 solely focused on infertile woman and 10 studies focused on infertile couple’s marital satisfaction, sexual satisfaction and marital relationships. A summary of the review is given in table I.
Due to variations in research protocols there were differences in sample sizes. The sample size in studies on infertile couples, ranged from 12 to 385; and in the studies on infertile individuals, the sample sizes ranged from 100 to 1017. The instruments were valid and reliable for the assessment of marital satisfaction in all of the reviewed studies. The most reported demographic variables were age, education, economic status, and duration of the marital relationship. Frequently represented clinical variables were type of infertility, time interval ever since diagnosis and treatment type.
The Sway of Marital Satisfaction
In the studies pertaining to infertility, marital discontent is increasingly reported due to the impact of infertility per se, and the relevant need of intervention to be provided during the process of infertility treatment. The purpose of this scoping review is to provide an overview of studies that addressed the impact infertility has on marital satisfaction of the couples.
In all of the selected studies, we found very few studies on infertile males’ marital satisfaction. The findings indicated that Infertile males had signiûcant negative effect on their sexual functioning. (Lee & Sun, 2000). Male infertility was found to have signiûcant negative effect on men’s sexual functioning. (Drosdzol & Skrzypulec, 2009).
Regarding marital satisfaction in infertile females 7 relevant studies were identified,
Prevalence of sexual dysfunction in infertile women was higher than in the fertile control group. specific domains that appeared to be most impacted were desire, arousal and orgasm. The rate of women who had reported presence of a sexual problem in male partner were significantly higher in the infertile group than the fertile group. The sexual dysfunction in women who were infertile was found to be associated with duration of marriage, duration of infertility, partner’s age, duration of treatment and frequency of intercourse (Oskay et al., 2010). In a Case control study by Wang in 2007 in China: 100 infertile women and a control group of 100 fertile women proved that infertility and in-vitro fertility treatment had a negative impact on the level of stress in the women’s marital quality. In a study using ENRICH Marital Inventory The stresses associated with infertility and In-vitro fertilization treatment had a negative impact on Chinese women’s marital quality (Wang et al. 2007).
A Longitudinal cohort study of 5 years done among 275 men and 272 women in Germany proved that satisfaction declined for both sexes in the partnership-related domains. Women were more affected than men. Satisfaction in all areas decreased dramatically. statistically significant difference was found in long-term satisfaction across men and women (Schanz et al, 2011). But in contradiction to this Amiri (2016) in a quantitative comparative study among infertile woman found that fertility status does not decrease marital satisfaction. It suggests that Since marital satisfaction was found to be moderate, sex education in schools, universities, for marrying people and sexual counseling for the couples can lead to improved sexual satisfaction.
The study that explored The issue of infertility and sexual function in Turkish women revealed that
DISCUSSION
Infertility carries along many complications such as unhappiness, sorrow, insomnia, stress, increase/decrease in appetite, social stigmatization, being exposed to curious questions about having a child, avoiding being in places with children, increase in the smoking habit, losing privacy of sexual life, having sexual intercourse in a planned way solely for the purpose of reproduction not of pleasure, interruption in work life, deterioration in family relations, and high cost of treatment expenses. Infertility and its treatment have effects on marital relationship. These effects speckled depending on the gender, the quality of the relationship and the stage of infertility process. (Onat et al, 2011)
The risk factors of marital dissatisfaction in infertility include; age over 30, , female sex, lower education level, diagnosis of male infertility and infertility duration of 3-6 years. (Drosdzol et al. 2009). While Keramat in 2013 quantified that the Quality of life status in infertile couples is directly associated with their social support, self-esteem, marital satisfaction and sexual satisfaction. On the contrary one study showed that shared stress of infertility may even stabilize marital relationships. (Reporaki et al. 2007) Moong in 2014 stated that infertile couples reported poor marital adjustment, sexual function and quality of life compared with fertile couples. Healthcare providers for infertile women should screen depressed women and help support infertile women from negative values for marriage depression. It is also necessary to include interventions for maintaining and enhancing the intimacy of couples during infertility treatment. (Kim et al,2018) A study in Poland revealed that Male infertility had the most signiûcant negative effect on men’s sexual functioning (Drosdzol & Skrzypulec, 2009) while in china the wives were less satisûed than their husbands with their marriage due to infertility. (Lee & Sun, 2000).
Infertility in women, has a diverse impact on multiple dimensions of health and functioning of infertile couples such as martial adjustment, Quality of life and sexual functioning. (Valsangkar et al, 2011). The prevalence of sexual problem and sexual dysfunction among infertile women is signiûcantly higher when compared to the fertile group. (Oskay et al., 2010). Infertility and Invitro fertilization treatment has a negative sway on the level of stress in the women’s marital quality (Wang et al,2007) A Longitudinal cohort study identified that women were more effected than men who were infertile and satisfaction decreased dramatically over five years. (Schanz et al, 2011) Various aspects of marital satisfaction among women will influence determinants of fertility adjustment, such as Emotional Intimacy, Sexuality and Communication/Conflict. (Ferreira et al, 2015) All dimensions of sexual function were found to be lower in infertile women in Iran compared with fertile women. (Direkvand et al,2015).
Psychological interventions, especially those emphasizing coping-skills and training stress management, have been shown to have beneficial effects for infertility patients. Further research is needed to develop effective psychosocial interventions. (Cousineau et al, 2007) Holding consultation programs and more studies are necessary for improving the quality of life and promoting sexual satisfaction and marital satisfaction in infertile couples. (Masoumi et al, 2016). Effective counseling, reassurance and measures to reduce the impact of the condition on marital and sexual life, overall quality of life are needed to impart a holistic treatment in infertility. This can be achieved in conjunction with treatment regimens by clinicians to provide a rounded approach in alleviation of the condition reducing the stress in infertile couples and helping them cope better. (Valsangkar et al, 2011).
While retrieving the literature most studies were predominately focusing on medical issues only a few studies explored the marital relationship aspects of infertile couples and the need for psychosocial interventions. It is Obvious that further research is needed in this area. The reviewed papers were confined to English so we could have missed some relevant non-English language studies. Even though all studies were selected according to inclusion criteria there may be still some bias due to the lack of a second, independent reviewer. Given these methodological confinements, it is imperative to consider all parts of the review while assessing their applicability.
CONCLUSION
Seventeen articles were included in this review. The results showed that infertility affected couples in the aspect of marital relationships and satisfaction. There is evidence that infertility has a negative effect on the marital satisfaction and sexual relationships of couples, the stresses associated with infertility and related treatment had a negative impact on marital quality. It was identified that infertility, regardless of which gender experiences it, brought along many problems such as unhappiness, stress, losing privacy of sexual life, having sexual intercourse. Infertility and its treatment have effects on marital relations and Quality of life. The effects varied depending upon the stage of infertility process, gender, and the quality of the relationship.
The quality-of-life was found to be generally lower for infertile couples than for the fertile couples. Severe symptoms of depression and anxiety was found among the infertile couples. In developing countries women carry the largest burden of suffering related to infertility. All these studies identify that the wellbeing of an infertile couple is truncated. The studies also verify that infertile couples are in need of psychosocial interventions; thus, establishing a need for psychosocial interventions.
LIMITATIONS AND FUTURE DIRECTIONS
This study is exploratory, and as such, its results must be interpreted with great caution. Its limitations include the small sample size and the low statistical power to detect differences between the three groups, and to predict proper classification. Future studies will also need to evaluate the measurement of object representation complexity variable as it was applied here, as well as the relationship patterns.
Nonetheless my preliminary findings are in general agreement with previous work on personality organization levels using the original CCRT method (Perry, 2004), and they are consistent with the general notion that patients with different disorders have different internal relationship patterns. I support the thesis that relationship patterns might be related to personality organization levels, and that object representation complexity might be a good predictor of psychological health – especially for distinguishing PPO and NPO from BPO. The empirical validation and clinical significance of the findings that we have derived now need to be further researched and verified to establish the contents findings as facts.
REFERENCES
Amiri, M., Sadeqi, Z., Hoseinpoor, M. H., & Khosravi, A. (2016). Marital Satisfaction and Its Influencing Factors in Fertile and Infertile Women. Journal of Family & Reproductive Health, 10(3), 139–145.
Bagarozzi, D. A. (2014). Enhancing Intimacy in Marriage: A Clinician’s Guide. Routledge.
Cousineau, T. M., & Domar, A. D. (2007). Psychological impact of infertility. Best Practice & Research Clinical Obstetrics
& Gynaecology, 21(2), 293–308. https:// doi.org/10.1016/j.bpobgyn.2006.12.003
Direkvand-Moghadam, A., Delpisheh, A., & Direkvand-Moghadam, A. (2015). Effect of Infertility on Sexual Function: A Cross-Sectional Study. Journal of Clinical and Diagnostic Research: JCDR, 9(5), QC01– QC03. https://doi.org/10.7860/JCDR/ 2015/11148.5934
Drosdzol, A., & Skrzypulec, V. (2008). Quality of life and sexual functioning of Polish infertile couples. The European Journal of Contraception & Reproductive Health Care, 13(3), 271–281. https://doi.org/ 10.1080/13625180802049187
Ferreira, M., Antunes, L., Duarte, J., & Chaves, C. (2015). Influence of Infertility and Fertility Adjustment on Marital Satisfaction. Procedia – Social and Behavioral Sciences, 171, 96–103. https://doi.org/10.1016/ j.sbspro.2015.01.094
Gadalla, A., Nasreldin, M., Mostafa, T., Ahmed, A.,
& Eid, A. (2011). Psychosexual satisfaction of infertile couples due to male factor infertility. Human Andrology, 1(2), 51–56. h t t p s : / / d o i . o r g / 1 0 . 1 0 9 7 / 01.XHA.0000399431.64941.67
Kardan-Souraki, M., Hamzehgardeshi, Z., Asadpour, I., Mohammadpour, R. A., & Khani, S. (2016). A Review of Marital Intimacy-Enhancing Interventions among Married Individuals. Global Journal of Health Science, 8(8), 74–93. https:// doi.org/10.5539/gjhs.v8n8p74
Karimi, S., Hasani, M., Soltani, Z., Dalvand, M. R.,
& Zohdi, M. H. (2012). Effects of Communication Skills Training on Increasing Intimacy between Male Teachers and their Spouses: A Case Study in Baane City. /paper/Effects-of-Communication-Skills-Training-on-between-Karimi-Hasani.
Kim, M., & Kim, H. S. (2018). Mediator Effect of Marital Intimacy on the Relationship between Depression and Marital Satisfaction of Infertile women. Journal of Korean Public Health Nursing, 32(1), 96–108. https://doi.org/10.5932/
JKPHN.2018.32.1.96
Lee, T. Y., Sun, G. H., & Chao, S. C. (2001). The effect of an infertility diagnosis on the distress, marital and sexual satisfaction between husbands and wives in Taiwan. Human Reproduction (Oxford, England), 16(8), 1762–1767. https://doi.org/ 10.1093/humrep/16.8.1762
Masoumi, S. Z., Garousian, M., Khani, S., Oliaei, S. R., & Shayan, A. (2016a). Comparison of Quality of Life, Sexual Satisfaction and Marital Satisfaction between Fertile and Infertile Couples. International Journal of Fertility & Sterility, 10(3), 290–296.
Masoumi, S. Z., Garousian, M., Khani, S., Oliaei, S. R., & Shayan, A. (2016b). Comparison of Quality of Life, Sexual Satisfaction and Marital Satisfaction between Fertile and Infertile Couples. International Journal of Fertility & Sterility, 10(3), 290–296.
Monga, M., Alexandrescu, B., Katz, S. E., Stein, M., & Ganiats, T. (2004). Impact of infertility on quality of life, marital adjustment, and sexual function. Urology, 63(1), 126–130. https://doi.org/10.1016/ j.urology.2003.09.015
Onat, G., & Beji, N. K. (2012). Marital Relationship and Quality of Life Among Couples with Infertility. Sexuality and Disability, 30(1), 39–52. https://doi.org/10.1007/s11195-011-9233-5
Oskay, U. Y., Beji, N. K., & Serdaroglu, H. (2010). The Issue of Infertility and Sexual Function in Turkish Women. Sexuality and Disability, 28(2), 71–79. https://doi.org/ 10.1007/s11195-010-9158-4
Repokari, L., Punamäki, R.-L., Unkila-Kallio, L., Vilska, S., Poikkeus, P., Sinkkonen, J., Almqvist, F., Tiitinen, A., & Tulppala, M. (2007). Infertility treatment and marital relationships: A 1-year prospective study among successfully treated ART couples and their controls. Human Reproduction, 22(5), 1481–1491. https://doi.org/ 10.1093/humrep/dem013
Schanz, S., Reimer, T., Eichner, M., Hautzinger, M., Häfner, H.-M., & Fierlbeck, G. (2011). Long-term life and partnership satisfaction in infertile patients: A 5-year longitudinal study. Fertility and Sterility, 96(2), 416–421. https://doi.org/10.1016/ j.fertnstert.2011.05.064
Tao, P., Coates, R., & Maycock, B. (2012). Investigating Marital Relationship in Infertility: A Systematic Review of Quantitative Studies. Journal of Reproduction & Infertility, 13(2), 71–80.
The Issue of Infertility and Sexual Function in Turkish Women | Request PDF. (n.d.). Retrieved March 19, 2020, from https:// www.researchgate.net/publication.
Ulbrich, P. M., Coyle, A. T., & Llabre, M. M. (1990). Involuntary childlessness and marital adjustment: His and hers. Journal of Sex & Marital Therapy, 16(3), 147–158. https:/ /doi.org/ 10.1080/00926239008405261
Valsangkar, S., Bele, S., Bodhare, T., & Sai, S. (2011). An evaluation of the effect of infertility on marital, sexual satisfaction indices and health-related quality of life in women. Journal of Human Reproductive Sciences, 4(2), 80. https://doi.org/10.4103/0974-1208.86088
Wang, K., Li, J., Zhang, J. X., Zhang, L., Yu, J., & Jiang, P. (2007). Psychological characteristics and marital quality of infertile women registered for in vitro fertilization-intracytoplasmic sperm injection in China. Fertility and Sterility, 87(4), 792–798. https://doi.org/10.1016/ j.fertnstert.2006.07.1534
WHO | Infertility definitions and terminology. (n.d.). WHO; World Health Organization. Retrieved March 19, 2020, from http:// www.who.int/reproductivehealth/topics/ infertility/definitions/en/
WHO | Infertility is a global public health issue. (n.d.). WHO; World Health Organization. Retrieved March 19, 2020, from http:// www.who.int/reproductivehealth/topics/ infertility/perspective/en/
Conflict of interest: None
Role of funding source: None


